Migraine: More Than a Headache, It’s a Neurological Experience
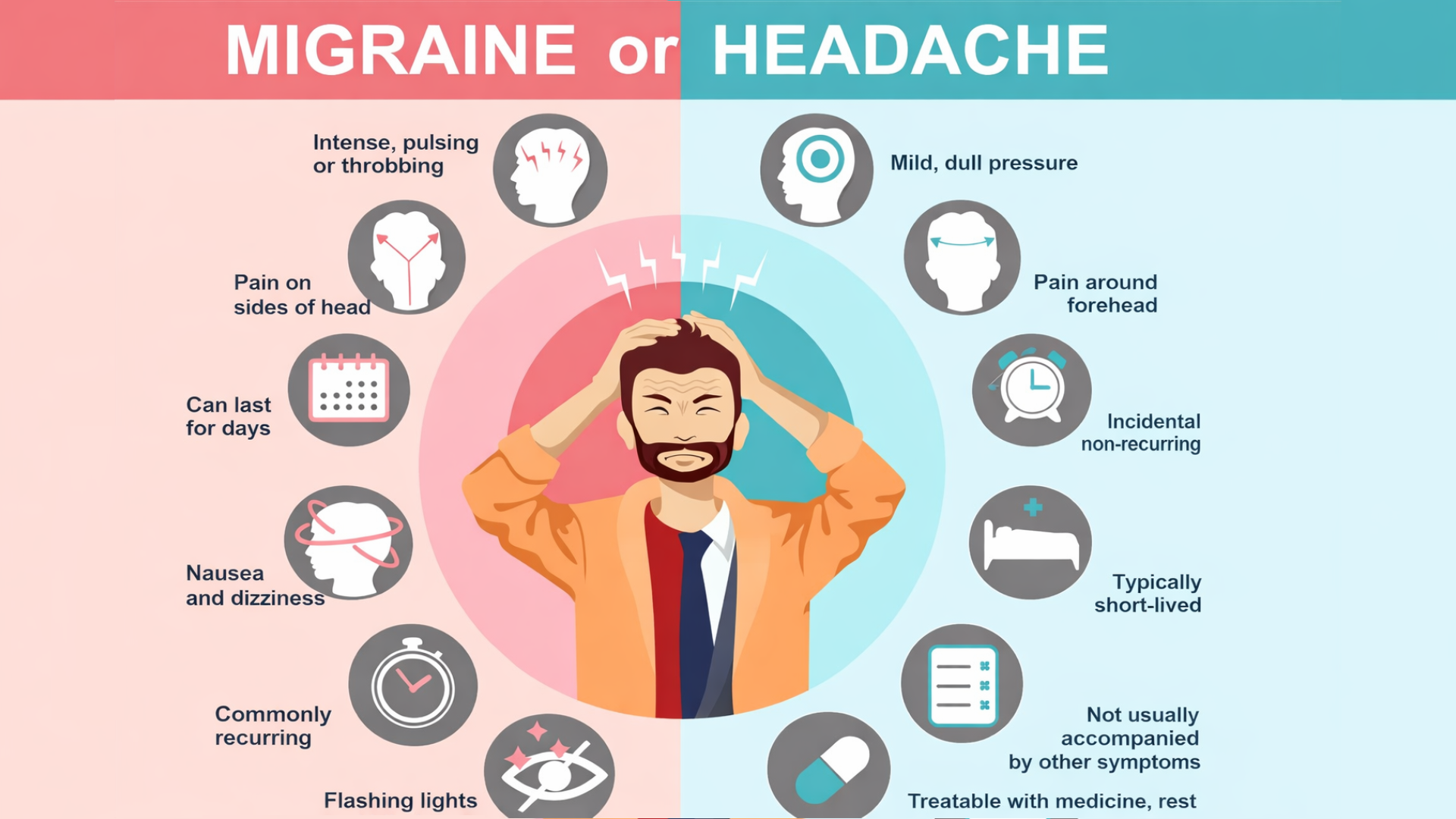
A migraine is often considered “just a severe headache or a bad headache.”
But one who has experienced migraine knows the truth—a migraine takes over your senses, your thoughts, and sometimes your entire day.
Migraine is a complex neurological disorder, not a sign of weakness, stress, or poor pain tolerance.
What Exactly Is a Migraine?
A migraine is a brain-based condition involving abnormal nerve signaling, chemical changes, and altered blood flow in the brain. It typically presents as recurrent attacks rather than a constant problem.
Unlike common headaches, migraines affect how the brain processes pain and sensory information.
The Many Faces of Migraine
Migraine do not look the same in everyone. It can appear as:
- Migraine without aura – the most common form
- Migraine with aura – involving temporary visual, sensory, or speech disturbances
- A Chronic migraine – The headache may be on and off for around 15 or more days a month, with typical migraine features on many of those days,
- Silent migraine – aura symptoms without head pain
This variability is one reason migraines are frequently misunderstood or misdiagnosed.
What Does a Migraine Attack Feel Like?
Migraine pain is often:
- Throbbing or pulsating
- Located on one side of the head, though it may spread
- Moderate to severe in intensity
- Worsened by physical activity
But pain is only one part of the story. Migraines commonly include:
- Nausea or vomiting
- Sensitivity to light, sound, or smell
- Difficulty concentrating
- Extreme fatigue
For many, even normal conversation or light can feel unbearable.
Understanding the Migraine Phases
A migraine attack may unfold in stages:
1. Prodrome (Hours to Days Before)
Subtle warning signs appear:
- Mood changes
- Food cravings
- Neck stiffness
- Frequent yawning
2. Aura (In Some People)
Temporary neurological symptoms such as:
- Flashing lights or zigzag lines
- Blind spots
- Tingling in the face or hands
- Speech difficulty
Aura symptoms are reversible but can be alarming.
3. Headache Phase
The main migraine attack occurs, lasting 4 to 72 hours if untreated.
4. Postdrome
After the pain subsides, many feel mentally foggy, drained, or unusually sensitive—often called a “migraine hangover.”
What Triggers a Migraine?
Triggers vary widely and are highly individual. Common ones include:
- Hormonal changes
- Irregular sleep
- Skipping meals
- Dehydration
- Stress or emotional shifts
- Certain foods or alcohol
- Strong smells or bright lights
- Weather changes
Importantly, triggers do not cause migraine—they lower the threshold for an attack in a sensitive brain.
Why Migraine Is Often Genetic
Migraine tends to run in families. If one or both parents experience migraines, the likelihood increases. This genetic predisposition affects how the brain responds to stimuli, making it more excitable.
Managing Migraine: Beyond Painkillers
Effective migraine care is individualized and may include:
- Identifying personal triggers
- Lifestyle regulation (sleep, meals, hydration)
- Acute treatments to stop attacks early
- Preventive strategies for frequent migraines
Self-treatment without guidance can worsen long-term outcomes.
When Should You Seek Medical Advice?
Consult a doctor if:
- Headaches are frequent or disabling
- Pain is worsening or changing in pattern
- You miss work or daily activities
- Over-the-counter medicines are used regularly
- Neurological symptoms occur
Migraine is treatable—but only when recognized correctly.
Bottom Line
Migraine is not “in your head” in the way people mean it.
It is in your brain, involving complex neurological processes that deserve understanding and proper care.
Listening to your symptoms, learning your patterns, and seeking expert guidance can transform migraine from a life-disrupting condition into a manageable one.
